By Monica E. Oss, Chief Executive Officer, OPEN MINDS
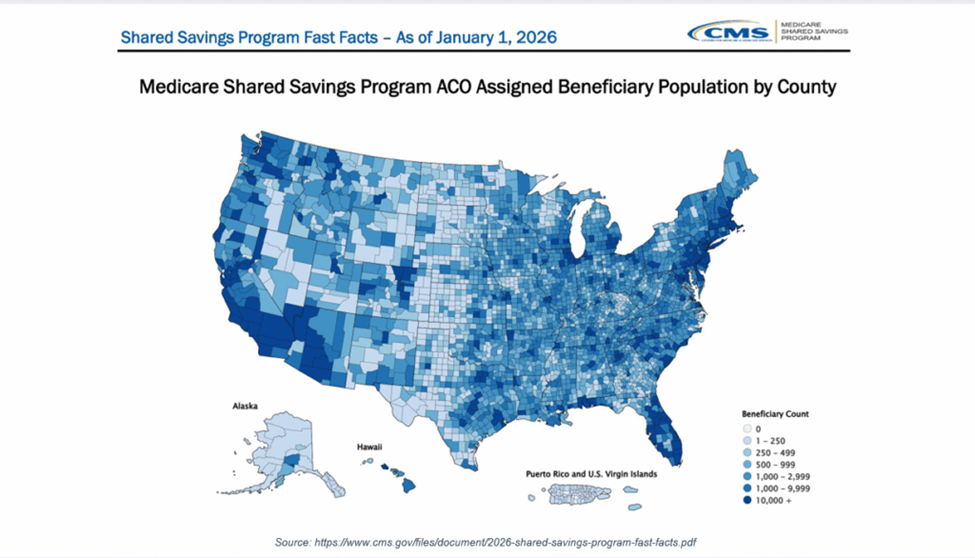
The coverage of Medicare beneficiaries by ACOs is on the upswing—as is the use of risk-based reimbursement models. As of January 2026, 14.3 million Medicare beneficiaries, approximately 23%, were enrolled in Accountable Care Organizations (ACOs), up from 13.7 million in 2025, according to a new CMS publication, 2026 Medicare Accountable Care Organization Initiatives Participation Highlights. This includes consumers whose clinicians are in the Medicare Shared Savings Program ACOs or are served by provider organizations participating in the CMS Innovation Center accountable care models and other CMS Innovation Center models.
For the 2026 performance year, CMS approved 134 applications for the Shared Savings Program, including 72 new ACOs and 62 renewing or reentering ACOs. This brings the total number of ACOs participating in the program to 511, up from 476 in 2025. These ACOs, with more than 700,000 clinicians and provider organizations, will serve 12.6 million consumers, a 12.3% increase from 2025.
The ACO REACH Model has 74 ACOs with 125,909 clinicians and provider organizations providing care to 1.7 million consumers. This model has 614 federally qualified health centers, rural health clinics, and critical access hospitals participating in 2026.
But the REACH model will be phased out, replaced by the recently announced Long-Term Enhanced ACO Design (LEAD) Model. The LEAD model will launch in 2027 at the conclusion of ACO REACH. LEAD will build on the REACH model but will include a broader mix of provider organizations, including those with specialized consumer populations and adding smaller, independent, and/or rural-based organizations. LEAD will focus on high-needs consumers, such as those dually eligible for Medicare and Medicaid, and those who are homebound or home limited.
Over the past few years, the financial impact of Medicare ACOs has improved along with the degree of risk sharing. In Performance Year 2024, the Shared Savings Program ACOs earned savings totaling $4.1 billion and saved Medicare $2.5 billion. And 82.8% of Shared Savings Program ACOs participated in the Advanced Alternative Payment Model—the highest percentage since 2012.
For community-based provider organizations, this tick upward in Medicare ACO enrollment and the expansion of risk-based contracting in Medicare has big implications. There are 62.7 million Americans enrolled in Medicare in 2024, roughly 18% of the population. And spending of this population was$1,118.0 billion in 2024, or 21% of total U.S. health care expenditures.
This large population is increasingly enrolled in models with value-based reimbursement. 35 million Medicare consumers are enrolled in Medicare Advantage health plans—almost 56%. Adding the 23% of the Medicare population enrolled in ACO programs, only 20% of consumers remain in the traditional fee-for-service program. The challenge for provider organization executive teams is to track the enrollment of consumers in their service area in Medicare Advantage plans and Medicare ACOs—and develop relationships with those value-based systems.