By Monica E. Oss, Chief Executive Officer, OPEN MINDS
There is significant body of research showing the impact of housing insecurity on health care costs—and the cost/benefit of providing housing-related services to high-needs populations. This research is summarized in publications like The Impacts Of Affordable Housing On Health: A Research Summary, The Health Cost Savings Of Quality Affordable Housing, and The Public Health Implications Of Housing Instability, Eviction, And Homelessness.
New research—Impact Of Housing Support Services For Medicaid Enrollees With Serious Mental Illness, Substance Use Disorder—takes another step in quantifying the costs of housing insecurity to the health care system. The analysis looked at the relationship between four housing support services provided in a Florida pilot—transitional housing support, tenancy support, peer support, and crisis management—and health care use and health outcomes of consumers with serious mental illness (SMI) or substance use disorder (SUD).
The researchers found that tenancy support and peer support were “particularly effective interventions.” Peer support was associated with a 20% reduction in ED use. Tenancy support services were associated with 51% lower odds of all-cause mortality: “We estimated that for every 15 enrollees receiving these services, one death was prevented.”
Some housing pilot services were associated with increased health care use. Transitional housing support services were linked to a 15% increased ED use. Crisis management was associated with a 45% increase in ED visits, a 41% increase in outpatient visits, and a 90% increase in psychiatric hospitalizations. The authors attributed this to identifying “newly surfaced unmet needs during housing transitions” and “stabilizing people in acute distress” and concluded that “Medicaid policy should prioritize high-value, data-driven housing interventions…Embedding these services within managed care contracts…offer a viable path for sustainability.”

The researchers concluded that “Medicaid policy should prioritize high-value, data-driven housing interventions and protect them from budget cuts. Embedding these services within managed care contracts and aligning them with broader care coordination strategies offer a viable path for sustainability.” Given the change in federal policy about health-related social needs, whether this will be possible in the years ahead is in question.
Another state—Arizona—has had success with integrating housing supports into health care for high-needs consumers. Through its Arizona Health Care Cost Containment System (AHCCCS), Arizona’s Medicaid program, the state has been providing health-related housing services since 2014. At The 2025 OPEN MINDS Strategy & Innovation Institute, Theresa Costales, M.D., chief medical officer at AHCCCS, Sandra Stein, M.D., chief medical officer of Banner Health Plans, and Shar Najafi-Piper, Ph.D, Chief Executive Officer of Copa Health, provided an overview of the state’s housing initiatives and its new Housing & Health Opportunities Program (H2O Program), in the session Innovations In Medicaid Funding To Advance Whole Person Care: The Arizona H2O Case Study.

The AHCCCS Housing Program (AHP), using a Housing First model, provides permanent supportive housing through units managed by both behavioral health provider organizations and community landlords. Members are expected to pay up to 30% of their income toward their rent while the balance is subsidized by the AHP. AHP funding is also available for housing-related supports and payments such as deposits, move-in assistance, eviction prevention, and damages related to member occupancy, as well as a wraparound services.
For the 2,472 members enrolled in AHP as of 2020, ACCCS found significant cost offsets. There was a 30% reduction in ED visits, a 44% drop in inpatient admissions, and $5,563 average cost savings per member per month.
Despite AHP’s success, AHCCCS still had about 30,000 members identified as homeless, 75% with at least one SUD-related encounter, with an average cost of around $23,000 per person per year. In response, AHCCCS applied for the 1115 waiver to create the Housing and Health Opportunities (H2O) program to complement AHP. Solari and Banner Health Plans serve as program administrators, with the demonstration period running through November 2027. Banner Health is responsible for network management; billing and claims; fraud, waste, and abuse; and contracting.
In response, AHCCCS applied for the 1115 waiver to create the Housing and Health Opportunities (H2O) program to complement AHP. Solari and Banner Health Plans serve as program administrators, with the demonstration period running through November 2027. Banner is responsible for network management; billing and claims; fraud, waste, and abuse; and contracting.
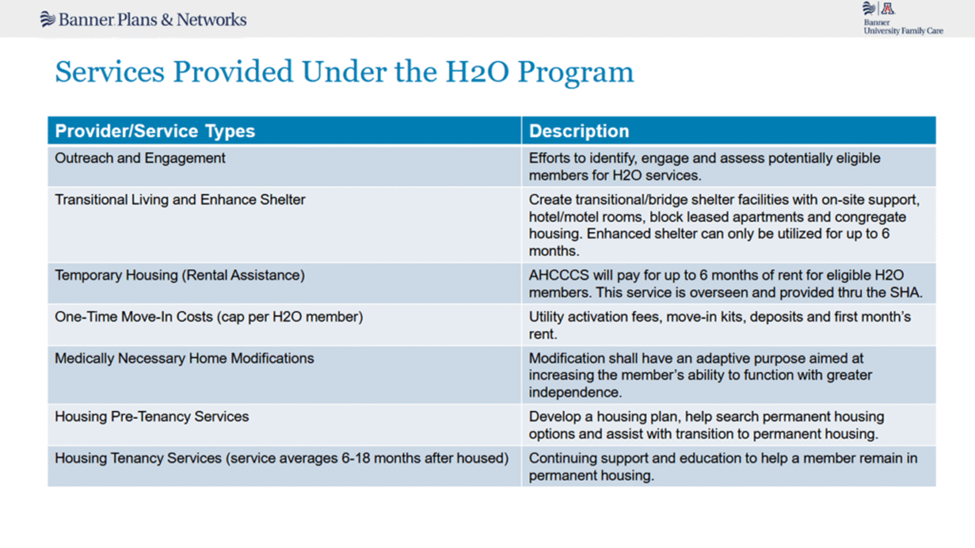
H2O provides transitional living services for a AHCCCS members who are homeless or at risk of homelessness and who have SMI and either a chronic health condition or are scheduled for release from a correctional facility or released in the last 90 days. This includes hotels, motels, block-leased apartments, and congregate housing. H2O pays up to six months of rent and one-time move-in costs, such as utility activation, deposits, and first month’s rent. They also make any medically-necessary home modifications. Since 2024, 536 members have been designated for H2O, with 34 members successfully housed as of mid-2025.
Program staff work with members to develop individualized housing plans that evolve as needs change, said Sandra Stein, M.D., chief medical officer of Banner Health Plans. Housing services continue for six to 18 months after permanent housing placement, providing education and support to promote long-term stability.
According to Dr. Stein, individualized housing plans and support services continue up to six months after permanent housing placement, providing education and support to promote long-term stability. She noted that the six-month limit to transitional housing support is a challenge. “In a perfect world, it would be longer, but everybody is working together to address these challenges…We’re having a profound impact, one member at a time, one program at a time.” The future of housing supports in Medicaid over the next two years is in question. CMS has announced a new policy to eliminate funding for services addressing health-related social needs. And based on policy documents of the administration, programs using the ‘Housing First’ model will likely not receive continuing funding. But in this changing policy environment, CMS executives—and executives of Medicare Advantage and Medicaid health plans—will need to find an alternate path to improving the health and reducing the spend of unhoused consumers.
