By Monica E. Oss, Chief Executive Officer, OPEN MINDS
The fact that unaddressed health-related social needs (HRSNs) drive up total cost of care for payers and health plans is not “new news.” But a new study—Cross-Sectional Analysis Of Insurance Claims Shows Health Care Utilization And Costs Associated With Health-Related Social Needs (HRSNs) In An Urban Population—added to the evidence base, finding that consumers who screened positive for unmet HRSNs incurred nearly twice the care costs. Those consumers had more outpatient visits, emergency department visits, and medical inpatient hospitalization days compared to those who screened negative.
The analysis was focused on adult consumers (ages 21 to 65) enrolled in a Medicaid managed care plan in the greater New York City metropolitan are. The HRSNs of consumers were assessed using the Health Leads Social Needs Assessment.

Of the 4,432 consumers included in the study, 26.9% reported at least one HRSN and 73% reported no HRSNs. Their mean annual health care cost were $8,170, compared with $4,393, respectively—a difference of almost 50% ($3,777). The higher total cost was due to higher utilization: 3.65 more specialty visits, 1.08 more mental health visits, 0.86 more emergency visits, and 0.40 additional inpatient days annually.
We got a look at how two organizations are addressing consumer social needs in the session Addressing Health-Related Social Needs In Your Service Delivery: Strategies & Solutions at The 2025 OPEN MINDS Strategy & Innovation Institute. Marco Damiani, chief executive officer of AHRC New York City, and Nia Uhlenhake, family support and community outreach manager at Arizona Autism United, described two models designed to address these gaps.
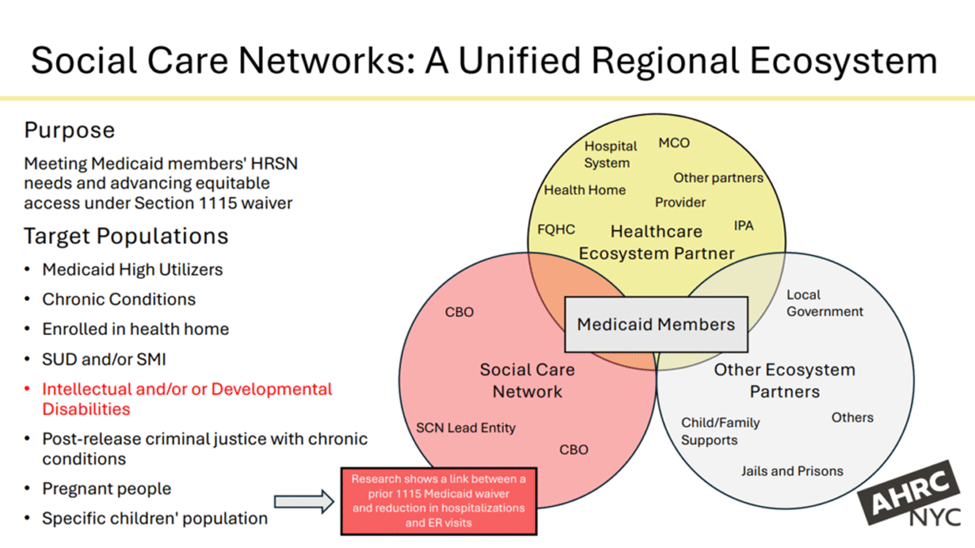
AHRC New York City, a $400 million non-profit that supports neurodivergent children and adults, developed an innovative Crisis Respite Transitional Residential Program (CRTP) in 2019 in partnership with New York City Health + Hospitals. The CRTP was created to address delayed hospital discharges for consumers with autism and I/DD due to lack of care transition options.
For consumers referred to the program, the AHRC NYC team provides an assessment and will make a CRTP crisis home available to facilitate discharge. And after the consumer is stabilized, AHRC NYC will work to find a long-term housing option, whether in a group living environment or other arrangement. Throughout the process, the AHRC NYC team will continue to provide services and supports, including psychiatric care, medication, and oral health care.
To date, around 45 people have been supported through CRTP. including 58% with autism, 20% with moderate I/DD, and 62% with a psychological diagnosis. Twenty-two percent were in the hospital for 50 to 99 days and 24% stayed in respite care for 20 to 49 days. With the success of the program, the New York State Office of Mental Health has invested $85 million over the next five years to replicate the model statewide.
Ms. Uhlenhake spoke about Arizona Autism United’s Clinical Family Coaching (CFC), an innovative program that helps train parents and caregivers of consumers with autism to remain in their homes. The training is focused on those consumers with challenging behaviors such as self-injury, physical aggression, and elopement.

In the family coaching program, the clinical team meets with the family twice a week for two to three hours. The coaching blends applied behavior analysis, parent management training, behavioral skills training, and acceptance and commitment therapy. The program is typically nine months but can vary based on the family. And the team can step back in after a family graduates if other behaviors have developed.
The consumer families’ evaluations of the program have been very positive according to Ms. Uhlenhake—with 94% reporting it gives them relevant care information and connects them to people who understand the situation. They also report they feel less stress knowing the team is there to support them.
For other executives developing programs to address consumer HRSNs, the executives advised that the models need to be developed for supporting the whole family, and not just the individual. The problem behavior exists within the larger family dynamic, Ms. Uhlenhake said, and all family members should be engaged throughout the treatment journey. Mr Damiani added, “We need to understand those family systems and support them as well as we can.”
For payers and health plan executives looking at reducing the total cost of care, developing programmatic models to address the social determinants of health for the highest need consumers will continue to be a focus. As the study authors noted, “incorporating screening for and addressing HRSNs in clinical settings could identify high-risk patients earlier and allow for targeted social interventions that may prevent avoidable health care utilization.” But with recent changes in federal policy on reimbursement for HSRNs, health plans will become the arbiters of what types of HRSNs are reimbursed and how.
