By Monica E. Oss, Chief Executive Officer, OPEN MINDS
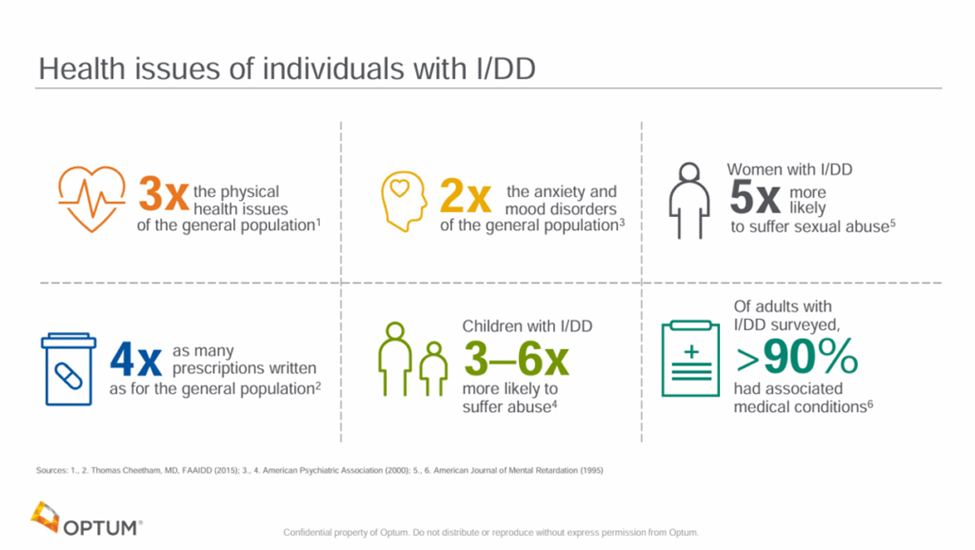
For consumers with intellectual/developmental disabilities (I/DD), my colleague agrees that whole person care models are increasingly the path to better health and lower total health care costs. This is due primarily to the functional effects of the disorders along with, sometimes hidden, co-occurring conditions. With regard to the latter, there are significant research findings that these consumers have three times more physical health problems than the general population and twice as many mental health disorders.
A new study, Anxiety, Depression, And Care Barriers In Adults With Intellectual And Developmental Disabilities, expands on this earlier data. Among adults with I/DD, 57% reported an anxiety diagnosis compared with 10.6% of adults without functional limitations. Similarly, 57% reported depression compared with 9.9% of other adults.
The good news is that some of these consumers are getting treatment. 42% use prescribed medications for anxiety and 38% use medication to treat their depression. The use of counseling or therapy is also common, with 41% of consumers reporting using these services in the past year. However, 18% reported delaying needed therapy or counseling due to cost and 9% reported not getting therapy at all due to cost.
The study authors point to a gap between need, utilization, and access to appropriate care. Adults with I/DD are engaging with the health care system at higher rates, but the type and intensity of care are not always aligned with the level of clinical need. They identify several factors driving this mismatch, including a shortage of clinicians trained in disability-informed psychotherapy, transportation barriers, long wait times, and difficulty navigating behavioral health systems, in addition to cost. At the same time, they note higher reliance on medication relative to therapy—suggesting that available treatment options may not be aligned with consumer needs.
The issue does not seem to be demand related; the issue is the ability to deliver care models that are designed for this population.

For additional insight, I turned to my colleague, OPEN MINDS Senior Associate, Rick Gutierrez, PhD, with a 25+ year career dedicated to working with individuals with I/DD. “The concerns reported or demonstrated by people with I/DD are often overlooked and attributed to their developmental disability, a phenomenon called diagnostic overshadowing. It is important that providers remain curious and get to the bottom of the concerns reported or demonstrated by people with I/DD.” Examples include an underlying medical condition like GERD, dental pain, or mental health conditions such as depression and anxiety that require behavioral health treatment. “A history of trauma can also be confused with other conditions due to a person’s communication vulnerability,” Dr. Gutierrez continued.
“There is an opportunity for provider organizations serving consumers with I/DD to expand their service model—both to include mental health and substance use disorder services and to address the chronic conditions typical in this consumer group. Too often, traditional behavioral health and primary care clinicians have not received sufficient training and supervision to serve those individuals that present with a neurodevelopmental disability. By focusing on building capacity, we will create a more equitable health care system for all.”
