By Monica E. Oss, Chief Executive Officer, OPEN MINDS
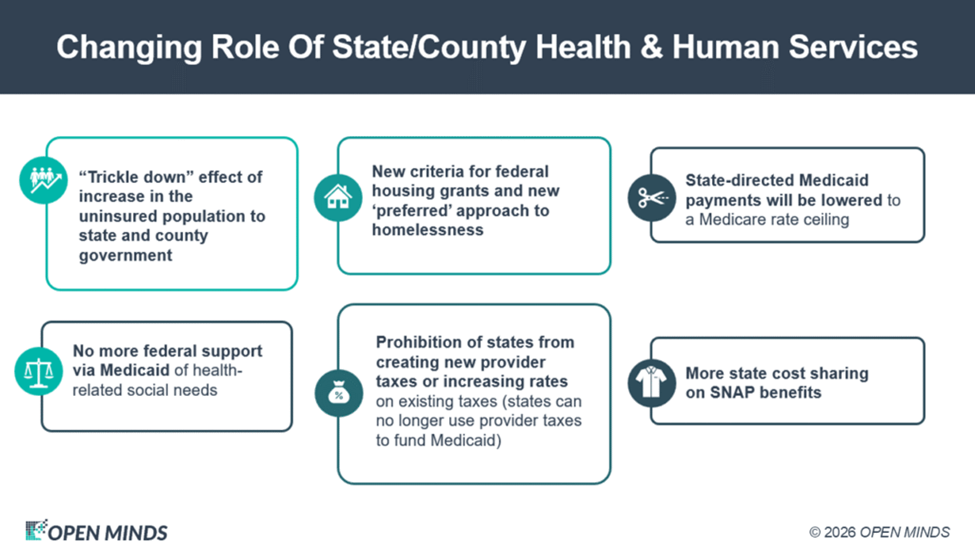
One big question for the year ahead is how state Medicaid plans will be affected by state budget problems. The changes in the last Congressional budget bill affect the financial tools that state governments have to fund Medicaid—particularly the prohibition of states from continuing with provider taxes to fund Medicaid and new limitations on state-directed payments to provider organizations.
There will also likely be more uninsured people to serve out of state coffers—an additional 10 to 16 million more. In addition, states will have to pick up more the costs of SNAP benefits and for meeting the health-related social needs of the population.
The strategic issue for health and human service provider organization executives is what decisions will states make to balance their books—and how those decisions will affect financial sustainability. We have an initial example of the potential impact of state budget problems on high-needs consumers: the Idaho Medicaid program made the decision to cut behavioral health services for people with serious and persistent mental illness (SPMI). In order to address the state’s budget deficit, Idaho Medicaid reduced rates for several services and coverage of assertive community treatment (ACT) and peer support services (among others) was eliminated.
This is a surprise given the robust literature on the cost/benefit of both ACT and peer support services. In one analysis, the introduction of peer support specialist staff at hospitals resulted in a reduction of 36% in the use of seclusion, a 48% reduction in the use of restraint, and a 56% reduction in hospital readmission rates.
In another, the North Carolina Results First Initiative, the North Carolina Department of Health and Human Services’ Adult Mental Health Section, and the North Carolina Office of State Budget and Management (OSBM) found that the introduction of peer support services resulted in a net benefit of $775 per person. This benefit of the peer support services was the result of both reduced psychiatric hospitalization and increase employment, with a return of $1.19 per dollar invested.
Looking ahead, there are at least 10 states with budget deficits and 11 with likely budget deficits. The challenge for governors and state legislators will be making the tough choices on state spending. The challenge for health and human service executives is educating state officials on the best path to improve the value of their health care investments.